Degenerative Disc Disease
Degenerative Disc Disease
What is degenerative disc disease?
Degenerative disc disease refers to changes in the discs in the spine, most often due to the aging process or to a spinal injury. Spinal discs are soft, compressible discs that separate the spine’s interlocking bones, or vertebrae. These discs serve as shock absorbers that enable the spine to bend and twist. While degenerative disc disease can happen anywhere in the spine, it typically affects the lumbar (lower back) region or the cervical (neck) region. Degenerative disc disease can also affect the thoracic (middle) region of the spine.
Changes in the discs can cause back or neck pain as well as other issues, including:
- Osteoarthritis, a type of arthritis associated with aging in which cartilage that protects and cushions joints breaks down.
- Spinal stenosis, the narrowing of the spinal canal, the open space in the spine that holds the spinal cord.
Appointment Information
For musculoskeletal-based back and spine conditions, call:
- Anesthesia Pain Management at 734-615-7246
- Physical Medicine & Rehabilitation at 734-936-7175
- Orthopaedic Surgery at 734-936-5780
- Neurosurgery at 734-936-7010
Comprehensive Spine Program
At the Comprehensive Spine Program, a nationally acclaimed team of back and spine care experts collaborates to deliver the most effective treatments, tailored to each patient, whether surgical or non-surgical.
What are the symptoms of degenerative disc disease?
For many individuals, degenerative disc disease may not cause any symptoms. Others, however, may experience back or neck pain and stiffness. The location of your pain depends on the affected disc:
- A degenerative disc in the neck area may result in neck or arm pain or numbness.
- A degenerative disc in the lower back may result in pain or numbness in the back, buttock or leg, difficulty walking and lack of balance or coordination.
- Occasionally, bowel and bladder control problems may occur with spinal cord stenosis or significant nerve compression.
How is degenerative disc disease diagnosed?
Our collaborative team begins by conducting a complete medical history and physical exam as well as a review of any symptoms, injuries or illnesses, previous treatment, or habits and activities that could be responsible for your pain.
Testing is done using the most advanced technologies and may include: Imaging such as X-rays, CT scans or MRI of the affected area. An EMG can also assess the electrical activity of the nerves and muscles. A discogram can evaluate back pain and help determine whether the degenerated disc is the cause of pain. After your diagnostic tests are completed, our specialists will talk with you about your treatment options.
How is degenerative disc disease treated?
Most cases of degenerative disc disease can be managed without surgery through our comprehensive pain program focused on interventional therapies. Non-surgical treatment is based on symptoms and is aimed at reducing pain and improving function.
Treatment may include:
- Physical therapy and exercises to help strengthen specific muscles to help the back heal and reduce the frequency of painful flare-ups.
- Pain management, including anti-inflammatory and pain medications, muscle relaxers, manual manipulation, steroid injections, electrical stimulation, radiofrequency ablation and heat/ice therapy.
- Traditional medicine combined with holistic therapies such as yoga, healing touch and acupuncture.
When symptoms related to disc degeneration don't improve with conservative treatment or if there is a progression of neurologic symptoms, surgery may be recommended. The goal of surgery is to relieve pressure on the nerves and stabilize the degenerated disc(s). Our spine specialists are skilled in the use of minimally invasive techniques that incorporate advanced navigation and robotics procedures, leading to faster recovery, less discomfort and shorter hospitalizations.
Treatment options include:
- Laminectomy: Removal of fragments of bone and soft tissue if spinal stenosis or significant nerve compression are involved. Depending on certain factors, this may be performed as a minimally invasive procedure or an open procedure. For more severe cases in which there is significant nerve compression, a laminectomy may be combined with a spinal fusion.
- Spinal Fusion: A procedure that reduces the movement in the damaged spine segment by permanently connecting two or more vertebrae using screws and rods to stabilize the spine. A bone graft is also typically performed using additional bone to fill in gaps between the vertebrae and stimulate the healing process.
- L5-S1 Anterior Lumbar Interbody Fusion: A procedure performed in the lower spine (typically L4-L5 or L5-S1) in which the disc is removed and a cage/interbody fusion is placed between the discs to help restore disc height and indirectly decompress the affected nerve(s). This procedure is performed through the abdomen versus the back, resulting in a smaller incision and quicker healing.
Patient Resources
- General Spine Surgery – Pre-operative education video for all spinal procedures
- Lumbar Laminectomy – Pre-operative educational video for a lumbar laminectomy
- Cervical Fusion – Pre-operative educational video for anterior and posterior cervical fusion
- Patient Education Booklet: Spine Surgery Pre-operative Patient Education
Locations
-
Back & Pain Center | Brighton Center for Specialty Care 7500 Challis Rd
Entrance 1, Level 1
Brighton, MI 48116-9416Get Directions -
Back & Pain Center | Burlington Building 325 E Eisenhower Pkwy
Floor 1
Ann Arbor, MI 48108-3364Get Directions -
Back & Pain Center | Canton Health Center 1051 N Canton Center Rd
Floor 1
Canton, MI 48187-5097Get Directions -
Back & Pain Center | Dexter Health Center 7300 Dexter Ann Arbor Rd Ste 110
Floor 1
Dexter, MI 48130-8598Get Directions -
Back & Pain Center | Northville Health Center 39901 Traditions Dr
Floor 1
Northville, MI 48168-9493Get Directions -
Back & Pain Center | West Ann Arbor Health Center-Parkland Plaza 380 Parkland Plaza Ste 210
Floor 1
Ann Arbor, MI 48103-6201Get Directions -
Spine Clinic | Brighton Center for Specialty Care 7500 Challis Rd
Entrance 1, Level 1
Brighton, MI 48116-9416Get Directions -
Spine Clinic | Chelsea Health Center 14700 E Old US Highway 12
Chelsea, MI 48118-1185Get Directions -
Spine Clinic | Northville Health Center 39901 Traditions Dr
Floor 1
Northville, MI 48168-9493Get Directions -
Spine Procedure Clinic | Burlington Building 325 E Eisenhower Pkwy Ste 100
Ann Arbor, MI 48108-3364Get Directions
Doctors

Ilyas Syed Aleem, MD
Clinical Associate Professor
Orthopedic Surgery

Rita N Ayyangar, MD
Clinical Professor
Pediatric Rehabilitation Medicine, Hospice & Palliative Medicine, Pediatrics, Physical Medicine & Rehabilitation

Rishi Rai Bakshi, DO
Clinical Associate Professor
Pain Medicine, Physical Medicine & Rehabilitation

Chad Michael Brummett, MD
Professor
Interventional Pain Medicine, Pain Medicine, Anesthesiology

Srinivas Chiravuri, MD
Clinical Associate Professor
Interventional Pain Medicine, Pain Medicine, Anesthesiology

Miles O Colwell, MD
Associate Professor Emeritus
Physical Medicine & Rehabilitation

Anita S W Craig, DO
Clinical Assistant Professor
Physical Medicine & Rehabilitation, Electrodiagnostic Medicine

Goodarz Micheal Golmirzaie, MD
Clinical Associate Professor
Interventional Pain Medicine, Pain Medicine, Anesthesiology

Anne Griffith Hartigan, MD
Clinical Assistant Professor
Physical Medicine & Rehabilitation, Electrodiagnostic Medicine

Paul Edward Hilliard, MD
Clinical Professor
Interventional Pain Medicine, Pain Medicine, Anesthesiology
Providers

Michael Edward Geisser, PhD
Professor
Clinical Psychology

Kathryn Elaine Matulich, NP
Advanced Practice Nurse
Nurse Practitioner

Maria Elise Powers, PA-C
Physician Assistant
Physician Assistant
News & Stories
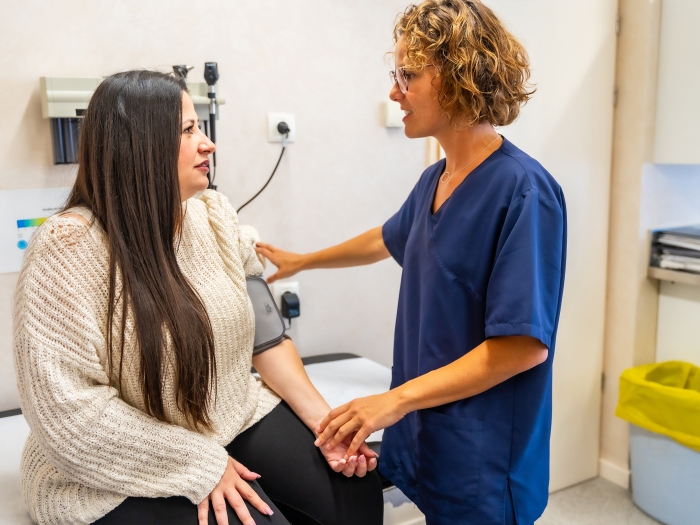
To reduce chronic pain, a new digital program could help

Half of newborns with severe spina bifida have trouble breathing during sleep

Finally hope after 9 surgeries for tethered cord syndrome

U-M to launch $16.5M NIH-funded project to advance personalized treatment for chronic lower back pain
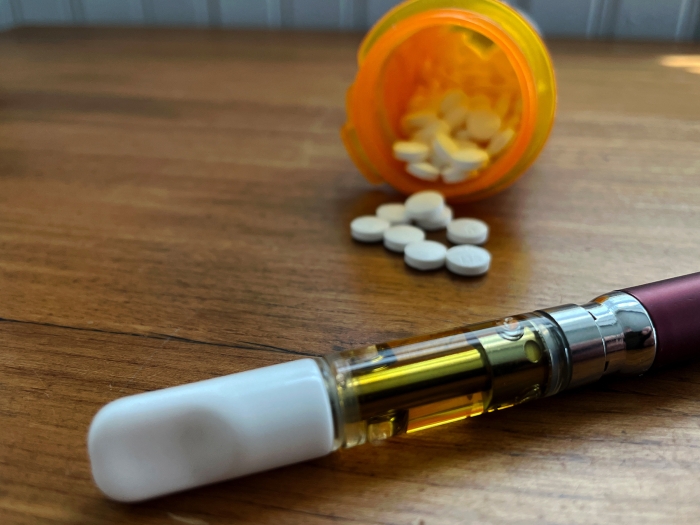
Primary care physicians are hesitant to accept chronic pain patients using opioids or cannabis








