
Most aortic aneurysms are abdominal aortic aneurysms. While small abdominal aortic aneurysms rarely rupture, they can grow very large without causing symptoms.
The typical size of the abdominal aorta is 2 to 3 centimeters – about the size of a quarter. An enlarged abdominal aorta is typically larger than 3 centimeters. Not all patients with an enlarged aorta require surgery but instead need regular surveillance and monitoring by their care team. This may include testing by CT scan or ultrasound imaging.
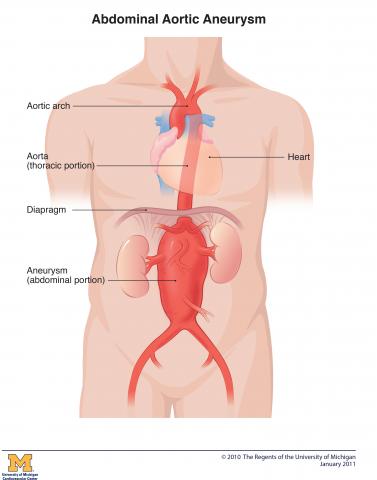
Symptoms and Causes
An abdominal aortic aneurysm typically produces no symptoms, but as the size of the aneurysm grows, abdominal and/or back pain may develop. Other symptoms may include pain radiating to the groin and a pulsating mass in the abdomen.
Although the exact cause of aortic aneurysms is unclear, risk factors such as smoking, in conjunction with diseases such as hypertension, increase the probability of developing the condition.
Diagnosis
Abdominal aortic aneurysms are often diagnosed as an incidental finding on an imaging study performed for some other reason. If an abdominal aortic aneurysm is suspected, testing may include:
- Abdominal ultrasound: Sound wave technology helps assess the aorta.
- Computerized tomography (CT) scan: Provides clear images of the aorta and detects the size and shape of an aneurysm.
- Magnetic resonance imaging (MRI): Imaging procedure to diagnose an aneurysm and determine its size and location.
AAA Treatment at University of Michigan Health
The Comprehensive Aortic Program at the Frankel Cardiovascular Center is one of the highest volume centers for abdominal aortic aneurysm in Michigan. With nine physicians dedicated to providing the highest quality of care for abdominal aortic aneurysms, our multidisciplinary program brings together a team of specialists to review complex cases and create the best treatment plan for each patient.
Our experts can manage complex aortic disease including abdominal aortic aneurysm and all conditions associated with it, including:
- Aortic infection
- Penetrating ulcer with pseudoaneurysm (false aneurysm)
- Post-traumatic aneurysm
- Small aneurysms with occlusion (blockage by clot)
Not all patients with abdominal aortic aneurysms require immediate surgical treatment. We provide comprehensive care and monitor the progression of the aneurysms until surgery becomes necessary.
In deciding whether to recommend surgery repair, a surgeon will consider the size of the aneurysm, its location, how fast it is growing, how complicated it is to repair, and the patient’s overall health.
Treatmet Options
To learn more, visit the Abdominal Aortic Aneurysm treatment page.
Patient Resources
Make an Appointment
Visit our Make an Appointment page for more information.

