Bladder Prolapse
Bladder Prolapse
What is bladder prolapse?
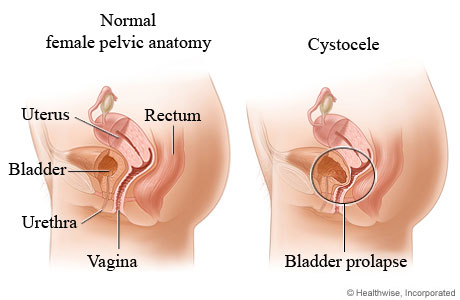
A bladder prolapse (cystocele) occurs when the tissues and muscles that hold the bladder in place get weak or damaged. This causes the bladder to move from its normal position and press against the front wall of the vagina. This is also called anterior vaginal wall prolapse.
Appointment Information
If you are a patient looking to receive kind and compassionate care at the leading urologic practice in Michigan, call 734–936–7030 to make an appointment.
What are the symptoms of bladder prolapse?
Sometimes a cystocele doesn't cause symptoms. But if you have symptoms, you may feel pressure from your bladder pressing against the vaginal wall. You may feel like something is falling out of your vagina. Or you may have urinary problems.
How is bladder prolapse diagnosed?
A cystocele can be hard to diagnose. If it doesn't cause symptoms, it may be found during a routine exam. Or, you may be aware that there's a problem. But you might not be quite sure where it is or what is causing it. If your doctor thinks you may have a cystocele, your doctor will ask you questions about your past and current health. This includes questions about your history of childbirth. Your doctor will also do a physical exam. This includes doing a pelvic exam. And it sometimes includes a rectal exam.
Your doctor may order tests, especially if the cystocele is causing urinary problems. These tests may include urodynamic tests or imaging tests, such as ultrasound or MRI. Urodynamic tests show how your body stores and releases urine.
Doctors use a system to rank the level of the bladder's prolapse. Finding the exact level of prolapse helps you and your doctor decide which treatments are most likely to work for the long term. One standard set of rankings uses "stages" of prolapse. It's based on how close the lowest part of the bladder is to the opening of your vagina. Your doctor checks this during your physical exam.
How is bladder prolapse treated?
A cystocele that doesn't cause symptoms may not need treatment. But if you have symptoms that bother you, you may want to think about treatment. Which treatment is best for you depends on how bad your symptoms are. And it depends on if you have other health problems. Other important factors are your age and sexual activity.
To treat a cystocele, your doctor may fit you with a pessary. This is a device that is placed into the vagina. It is removable—you can take it out and put it back in. It supports the area where the bladder presses down.
Exercises to strengthen the pelvic floor muscles may help relieve some symptoms of a cystocele. These are called Kegel exercises.
Surgery may be an option if your symptoms don't get better with other treatments. You may also choose surgery if you prefer it over other options. But if you are thinking about getting pregnant in the future, you may want to wait to have surgery. If you have surgery and then give birth through the vagina, the strain on your pelvic muscles may cause your bladder to prolapse again.
Locations
-
Obstetrics & Gynecology Clinic | Chelsea Professional Office Building Floor 1 Ste 101
Chelsea Multispecialty Clinic
Chelsea, MI 48118-1801Get Directions -
Obstetrics & Gynecology Specialty Clinic | Northville Health Center 39901 Traditions Dr
Floor 2
Northville, MI 48168-9493Get Directions -
Obstetrics & Gynecology Specialty Clinic | West Ann Arbor Health Center-Parkland Plaza 380 Parkland Plaza Ste 210
Floor 2
Ann Arbor, MI 48103-6201Get Directions -
Urology Clinic | Chelsea Professional Office Building Floor 1 Ste 101
Chelsea Multispecialty Clinic
Chelsea, MI 48118-1801Get Directions -
Urology Clinic | Northville Health Center 39901 Traditions Dr
Floor 2
Northville, MI 48168-9493Get Directions -
Women's Clinic | Von Voigtlander Women's Hospital 1540 E Hospital Dr
Floor 9
Ann Arbor, MI 48109-4276Get Directions
Doctors

John O De Lancey, MD
Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology

Pamela Susan Fairchild, MD
Clinical Associate Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology

Dee Ellen Fenner, MD
Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology

Priyanka Gupta, MD
Clinical Associate Professor
Female Pelvic Medicine & Reconstructive Surg, Urology, Female Pelvic Medicine & Reconstructive Surgery

Daniel McBurney Morgan, MD
Clinical Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology

Megan O'Brien Schimpf, MD, MHSA
Clinical Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology

Payton Claire Schmidt, MD
Clinical Assistant Professor
Female Pelvic Medicine & Reconstructive Surgery, Obstetrics & Gynecology
News & Stories
Urine-based test detects aggressive prostate cancer

How donor eggs helped one couple build the family they always hoped for

What causes infertility? A doctor answers common questions and clears up misconceptions

Insurance that covers male infertility procedures improves opportunities for family building

IVF insurance coverage varies greatly among larger employers
