
Primary hyperparathyroidism is a condition that causes elevated calcium levels (hypercalcemia) in the bloodstream, due to the parathyroid glands secreting too much parathyroid hormone (PTH). In a healthy body, when the calcium level is high, the PTH level should be very low or undetectable. The body doesn't need the parathyroid glands to produce any PTH when the calcium levels are high in the blood stream.
When the PTH level is above normal and the calcium level is also above normal, this is called primary hyperparathyroidism (or PHPT). It is by far the most common type of hyperparathyroidism, and in 85% of patients the disorder is caused by a single abnormal gland.
What Causes Primary Hyperparathyroidism?
Primary hyperparathyroidism is caused by abnormal growth of cells within the parathyroid gland. In most cases a single gland is involved, but 15-20% of the time multiple glands are abnormal. In 99% of cases, these are non-cancerous growths. Parathyroid cancers often present with very high calcium levels (often >13mg/dL) and have slightly different appearances on imaging studies. Parathyroid disease can be due to genetic abnormalities, passed from one family member to another. Genetic syndromes affecting the parathyroid glands include multiple endocrine neoplasia syndromes (MEN) I and IIA.
What Are the Symptoms of Primary Hyperparathyroidism?
Signs and symptoms of primary hyperparathyroidism can range from none or very mild to extremely serious. Measurable signs of abnormally functioning parathyroid glands may include:
- Brittle bones (osteopenia and osteoporosis) which can lead to fractures
- Kidney stones and decreased kidney function
- Increased acid secretion in the stomach with may lead to gastritis or ulcers
- Pancreatitis
- Heart disease
Some patients develop symptoms that can be difficult to determine if they are from parathyroid disease or other problems that can cause similar symptoms. These symptoms may include:
- Fatigue
- Depression
- Anxiety
- Insomnia
- Difficulty concentrating
- Difficulty with memory
- Generalized muscle aches and pains
- Frequent urination (especially at night)
- Constipation
How Is Primary Hyperparathyroidism Diagnosed?
Since the symptoms of primary hyperparathyroidism can be non-existent or very mild for a long time, the condition is often discovered as part of routine blood testing done at the time of a yearly routine physical examination or at the time of evaluation for another unrelated medical condition. If a patient goes to a physician already experiencing some of the above signs or symptoms, blood tests can be ordered to check for primary hyperparathyroidism. Common tests ordered to check for primary hyperparathyroidism include serum and/or ionized calcium, parathyroid hormone, basic metabolic panel, phosphorous, 25 hydroxy vitamin D, and 24 hour urine for calcium and creatinine.
How Do We Locate Abnormal Parathyroid Glands?
A number of different types of imaging studies may be used to locate abnormal parathyroid glands, but even if someone has the disease, an abnormal gland or multiple abnormal glands may not show up on the imaging study. Primary hyperparathyroidism is a biochemical (lab) diagnosis, so parathyroid surgery should not be dismissed if an abnormal gland is not identified by imaging. Often, the glands hide behind other structures and can’t be seen until structures can be moved out of the way during surgery.
The most common imaging studies obtained are ultrasound and sestamibi scans, but CT, MRI, and other types of imaging studies may also be ordered.
Parathyroid Ultrasound
Ultrasound uses sound waves to generate images. It is painless and can be performed in the office by your surgeon. Many times, if an obviously enlarged parathyroid gland is identified, no other imaging is necessary and a minimally invasive surgery can be performed.
Sestamibi Scan
Sestamibi scans are imaging studies done in the Nuclear Medicine area of the Radiology department.
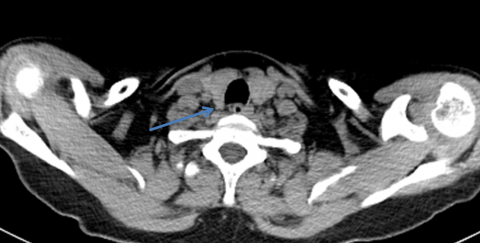
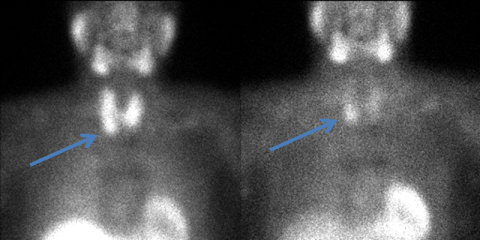
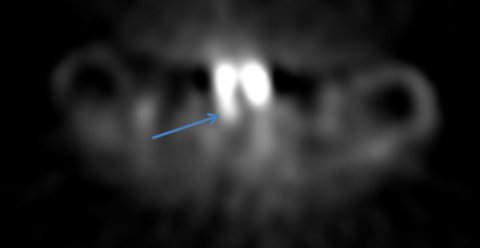
Sestamibi scans are performed by injecting a small amount of radioactive material into a vein. The radioactive tracer is initially taken up by both the thyroid gland and the parathyroid glands. The tracer is taken up to a greater extent and takes longer to leave a hyperfunctioning parathyroid gland than a normally functioning parathyroid gland allowing us to visualize it.
Pictures are taken twice—about 10-20 minutes after the tracer is injected and again 2 hours later. CT imaging is also done at the same time to better see the area of increased tracer uptake. This study can increase our ability to localize any abnormally functioning parathyroid adenomas. It is a routine procedure– all the patient has to do is lie still on a table for a few minutes.
