Aortic valve diseases can threaten your health and impact your quality of life. Our heart and vascular specialists at the University of Michigan Health Frankel Cardiovascular Center are skilled in diagnosing and treating diseases of the aortic valve.
We use innovative techniques and a unique team-based approach to help you feel better as quickly as possible.
Aortic Valve Disease Care at the Frankel Cardiovascular Center

At the Frankel Cardiovascular Center, you’ll find expert, patient-centered care. Our team approach brings together cardiologists, surgeons, radiologists, nurse practitioners, care coordinators and many others to offer patients:
- Access to leading experts in aortic valve disease: Our surgeons are among the top in the nation. They are continually developing new treatments and refining existing ones to improve patient outcomes.
- Enrollment in the latest clinical trials: As one of the nation’s largest aortic valve programs, we participate in clinical trials for medical device companies. This gives you access to treatments and devices that may not be available elsewhere.
- Personalized treatment planning: Our team meets weekly to review your case, evaluate your symptoms and identify treatment options. We then work with you to develop a treatment plan that is best for your condition and personal needs.
Types of Aortic Valve Disease
The aorta is the large blood vessel that carries oxygenated blood from the heart to the rest of the body. The aortic valve is located within the aortic root. This is where the aorta joins the left ventricle, or main pumping chamber, of the heart.
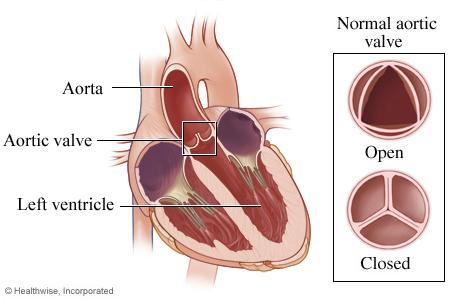
A healthy aortic valve has three leaflets that open as the left ventricle contracts to let blood flow. When the ventricle rests, the aortic valve shuts to prevent blood from flowing backward.
There are two main types of aortic valve disease:
- Regurgitation occurs when the aortic valve doesn’t close properly. This is also known as aortic insufficiency or a leaky aortic valve because it lets blood leak back into the heart.
- Stenosis is a narrowing of the aortic valve that restricts blood flow. It is caused by calcium buildup or scarring that damages the leaflets.
Both stenosis and regurgitation can cause the ventricle to work harder to pump blood. Left untreated, this can lead to an irregular heartbeat, cardiomyopathy (thickening of the heart muscle) and heart failure.
Causes of Aortic Valve Disease
Aortic valve diseases can be present at birth (congenital) or acquired later in life.
Bicuspid aortic valve is the most common genetic abnormality of the aortic valve. A bicuspid aortic valve has two leaflets instead of three. The valve may function well for many years or a lifetime. If stenosis develops or it becomes leaky, the valve may need repair or replacement. Find out more about bicuspid aortic valve.
Aortic valve disease can also be caused by:
- Age-related buildup of calcium that causes the valve to become narrow and stiff (stenosis)
- Heart conditions such as a prior heart attack or high blood pressure that can damage the aortic valve
- High-dose radiation from cancer treatment
- Infections such as rheumatic fever or infective endocarditis (an infection of inner lining of the heart that can also involve the heart valves)
Symptoms of Aortic Valve Disease
Many people with aortic valve disease do not experience any symptoms. As the disease progresses, you may notice a general decline in activity level. Other symptoms may include:
- Chest pain or tightness
- Dizziness, lightheadedness or fainting
- Fatigue, especially with activity
- Rapid or irregular heartbeat
- Shortness of breath or difficulty breathing when lying down
Diagnosing Aortic Valve Disease
At the Frankel Cardiovascular Center, our team will work with you to assess your symptoms and make an accurate diagnosis. You will have most of your tests done under one roof and frequently in one visit.
Diagnosing aortic valve disease starts with a health assessment, review of your medical history and physical exam. Your doctor will also listen to your heart for a whooshing sound (murmur), a sign of heart valve disease.
Other tests our doctors use to diagnose aortic valve diseases include:
- Cardiac computerized tomography (CT) scan: Creates a detailed image of your heart and valves using a special type of X-ray.
- Chest X-ray: Shows your aorta and calcium buildup on the aortic valve.
- Coronary angiography: Takes an X-ray of your heart and valves after a dye is injected into your heart through a catheter. A catheter is a thin tube that is inserted into a blood vessel in your arm or groin and guided to your heart.
- Echocardiogram: Produces a video of your heart and valves in action using ultrasound waves. For a closer look, your doctor may order a transesophageal echocardiogram (TEE). A small ultrasound probe is inserted into your esophagus (tube that runs from the throat to the stomach) to get detailed images of your aorta and upper heart chambers.
- Electrocardiogram (ECG): Tracks the electrical activity of your heart. An ECG can detect an irregular heartbeat and enlarged heart chambers.
- Exercise or stress ECG test: Measures how your heart responds to physical activity. If you cannot exercise, you can take a medication that mimics exercise.
Treating Aortic Valve Disease
At the Frankel Cardiovascular Center, you’ll receive care from a nationally recognized program. We’re nationally ranked for Cardiology and Heart Surgery by U.S. News & World Report Best Hospitals. We’ve also received top scores for abdominal aortic aneurysm repair, aortic valve surgery and transcatheter aortic valve repair (TAVR).
We offer treatments that range from nonsurgical to minimally invasive to open surgery:
Nonsurgical Treatments for Aortic Valve Disease
Not all patients with aortic valve disease will require surgery. Depending on your age, health, condition and symptoms, we may recommend nonsurgical treatments such as medications and lifestyle changes.
Your doctor may prescribe medications to:
- Improve cholesterol
- Lower blood pressure
- Prevent blood clots
- Reduce stress on the heart
While these medications don’t cure aortic valve disease, they can control your symptoms and prevent further damage.
We can also work with you to implement lifestyle changes that may improve your condition. You benefit from specialists who can help you quit smoking, improve your diet and be more physically active.
Transcatheter Aortic Valve Replacement (TAVR)
TAVR is a minimally invasive procedure for patients with severe aortic stenosis. In the past, TAVR was only approved for high-risk patients who were not candidates for open surgery. It is now approved for all patients.
During TAVR, the doctor uses a catheter to insert a replacement valve inside the diseased valve. Because the procedure is minimally invasive, you have a faster recovery and a lower risk of postoperative infection. Learn more about TAVR.
Open Aortic Valve Surgery
Though many patients prefer minimally invasive procedures, sometimes open surgery — in which the surgeon uses a larger incision to directly access the heart — is the best option. At the Frankel Cardiovascular Center, our outcomes for open surgery are among the best in the nation.
During open surgery, the aortic valve can be replaced or repaired. Patients with stenosis typically require valve replacement. Leaky valves can often be repaired or replaced. Because replacement valves have a limited lifespan, surgeons prefer to repair a diseased aortic valve if possible, especially in younger patients.
Replacement valves can be mechanical (manufactured) or made of biological tissue:
- Mechanical valves last longer, but you must take blood thinners for the rest of your life to prevent blood clots.
- Tissue valves are made of animal or human tissue. You don’t need to take blood thinners with this type of valve, but they have a shorter lifespan than mechanical valves.
Our surgeons have developed a reputation as leaders in aortic valve open surgery. Some of the specialized procedures they perform include:
David procedure (valve-sparing aortic root replacement): This procedure is used when an aortic aneurysm or dissection occurs near the aortic root, but the valve is healthy. The surgeon replaces the damaged root with a graft and reimplants the healthy valve in the new aortic root. This allows you to keep your aortic valve, which is more resistant to infection. It also eliminates the need to take blood thinners for life.
Ross procedure: The surgeon replaces the diseased aortic valve with the pulmonary valve (one of the other four heart valves). The pulmonary valve is then replaced with a tissue valve. The Ross procedure is often preferred for younger patients because the relocated aortic valve can grow with the child. This prevents the need for future surgeries. Read more about the Ross procedure.
Y-incision/rectangular patch aortic root enlargement: This procedure was developed at the Frankel Cardiovascular Center and is recognized globally as game-changing for patients who need a new aortic valve but have a small aortic root. The surgeon enlarges the aortic root and inserts a replacement prosthetic valve that is three to four sizes larger. The larger valve results in better blood flow and a better outcome if the valve must be replaced in the future.
Make an Appointment
To schedule an evaluation with a Frankel Cardiovascular Center physician, call 888-287-1082. Or visit the Make a Cardiovascular Appointment page to learn what to expect when you call us.
Physicians: To refer a patient, call M-Line at 800-962-3555.

