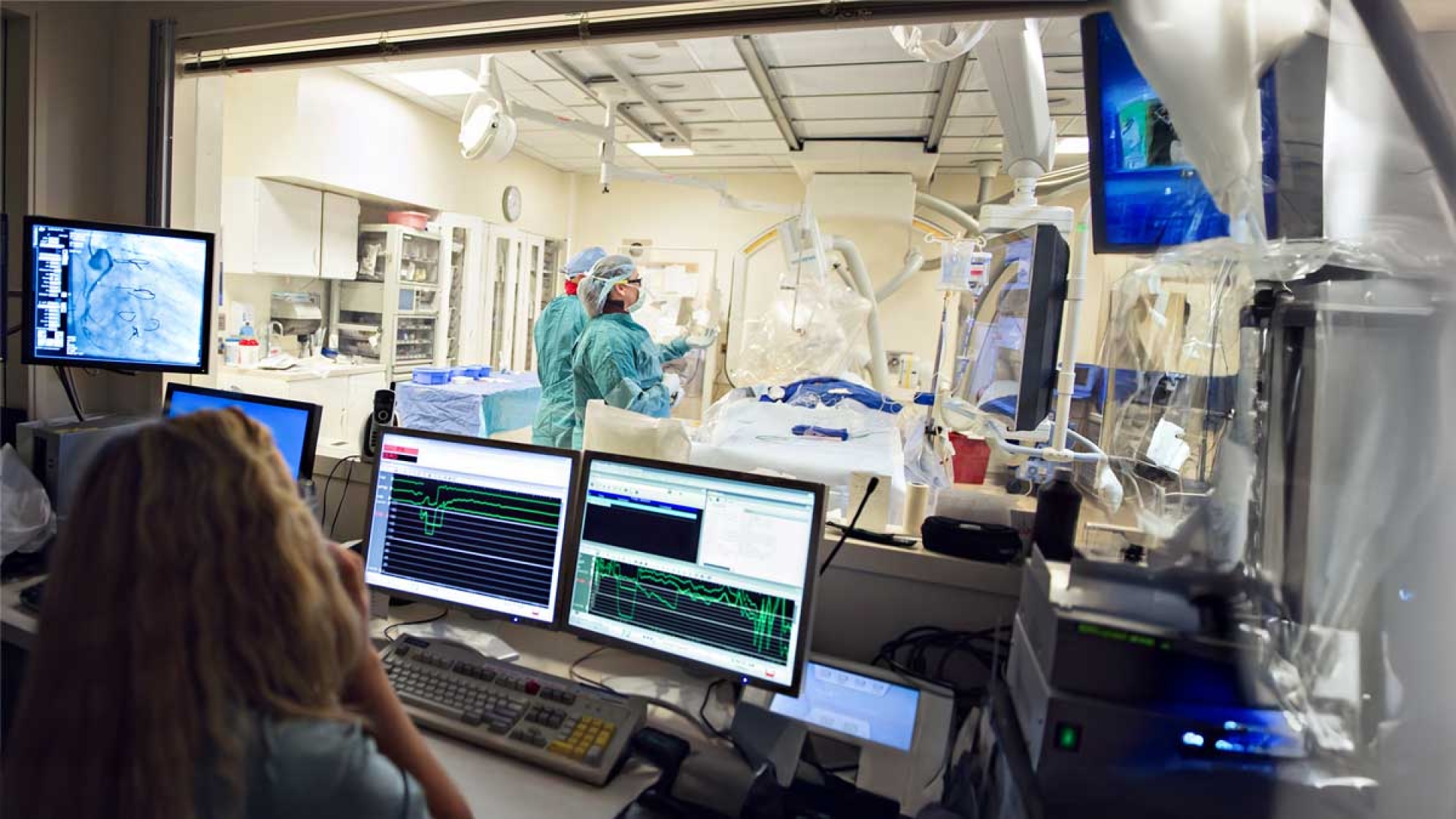
Radiology & Imaging
Radiologists and imaging specialists use advanced technology that allows specialists to see inside the body and diagnose or treat conditions.
Your Michigan Answer for Imaging Care
The first step to a diagnosis or treatment plan is often an image. Radiology and other imaging types help providers see your internal systems and make decisions about your care. Don’t settle for less than the highest possible standards.
We practice focused radiology for both adults and pediatrics. That means a board-certified, fellowship-trained specialist takes your images. This approach gives us a deeper understanding of what your provider needs to see. It also creates a more insightful foundation for your care. From our cancer and cardiovascular centers to our children’s hospital, great outcomes begin with great images. Learn more about pediatric radiology services.
Rest assured that we’re committed to using the lowest possible necessary radiation. Our CT scanners use state-of-the-art hardware and software tools to lessen your exposure. Every day, our researchers and engineers work to reduce that amount even more. Learn more about diagnostic radiology services.
Our new neuro-interventional suite is the first of its kind in the nation. This technology allows us to detect and treat strokes, aneurysms and rare conditions. Patients needing emergency procedures can get a diagnosis and surgery, all in the same room. This allows us to treat conditions that need life-saving, emergency care, faster. Learn more about interventional radiology services.
When an image can be a foundation for your care, don’t settle for less than U-M Health.