Top of the pageCheck Your Symptoms
Headaches
Overview
Headaches are one of the most common pain-related health problems in both children and adults. You may have a headache along with another minor health problem such as a sore throat, a cold, or a sinus problem.
Types of headaches
Most types of headaches usually aren't dangerous. Some headaches may occur again and again, such as:
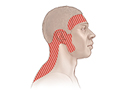
- Tension headaches. These are the most common type of headache. They are often caused by stress and emotional strain. Most adults have tension headaches from time to time, and everyone may have different areas of pain.
- Cluster headaches.
- Migraine headaches.
Common causes of headaches
Common causes of headaches may include:
- Stress.
- Skipping meals or not getting enough to eat.
- Sleeping too much or not enough.
- Alcohol use.
- Sinus problems.
- Getting too much or too little caffeine.
- Certain foods or drinks.
In rare cases, a headache may be a symptom of a serious illness or injury.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Check Your Symptoms
The medical assessment of symptoms is based on the body parts you have.
- If you are transgender or nonbinary, choose the sex that matches the body parts (such as ovaries, testes, prostate, breasts, penis, or vagina) you now have in the area where you are having symptoms.
- If your symptoms aren’t related to those organs, you can choose the gender you identify with.
- If you have some organs of both sexes, you may need to go through this triage tool twice (once as "male" and once as "female"). This will make sure that the tool asks the right questions for you.
Many things can affect how your body responds to a symptom and what kind of care you may need. These include:
- Your age. Babies and older adults tend to get sicker quicker.
- Your overall health. If you have a condition such as diabetes, HIV, cancer, or heart disease, you may need to pay closer attention to certain symptoms and seek care sooner.
- Medicines you take. Certain medicines, such as blood thinners (anticoagulants), medicines that suppress the immune system like steroids or chemotherapy, herbal remedies, or supplements can cause symptoms or make them worse.
- Recent health events, such as surgery or injury. These kinds of events can cause symptoms afterwards or make them more serious.
- Your health habits and lifestyle, such as eating and exercise habits, smoking, alcohol or drug use, sexual history, and travel.
Try Home Treatment
You have answered all the questions. Based on your answers, you may be able to take care of this problem at home.
- Try home treatment to relieve the symptoms.
- Call your doctor if symptoms get worse or you have any concerns (for example, if symptoms are not getting better as you would expect). You may need care sooner.
Neurological symptoms—which may be signs of a problem with the nervous system—can affect many body functions. Symptoms may include:
- Numbness, weakness, or lack of movement in your face, arm, or leg, especially on only one side of your body.
- Trouble seeing in one or both eyes.
- Trouble speaking.
- Confusion or trouble understanding simple statements.
- Problems with balance or coordination (for example, falling down or dropping things).
- Seizures.
Pain in adults and older children
- Severe pain (8 to 10): The pain is so bad that you can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain.
- Moderate pain (5 to 7): The pain is bad enough to disrupt your normal activities and your sleep, but you can tolerate it for hours or days. Moderate can also mean pain that comes and goes even if it's severe when it's there.
- Mild pain (1 to 4): You notice the pain, but it is not bad enough to disrupt your sleep or activities.
You can get dehydrated when you lose a lot of fluids because of problems like vomiting or fever.
Symptoms of dehydration can range from mild to severe. For example:
- You may feel tired and edgy (mild dehydration), or you may feel weak, not alert, and not able to think clearly (severe dehydration).
- You may pass less urine than usual (mild dehydration), or you may not be passing urine at all (severe dehydration).
Many prescription and nonprescription medicines and supplements can cause headaches. A few examples are:
- Medicines that contain hormones, such as birth control pills and hormone therapy for menopause.
- Medicines for erection problems.
- Caffeine (because of caffeine withdrawal).
- Some heart and blood pressure medicines.
- Vitamins.
Severe dehydration means:
- Your mouth and eyes may be extremely dry.
- You may pass little or no urine for 12 or more hours.
- You may not feel alert or be able to think clearly.
- You may be too weak or dizzy to stand.
- You may pass out.
Moderate dehydration means:
- You may be a lot more thirsty than usual.
- Your mouth and eyes may be drier than usual.
- You may pass little or no urine for 8 or more hours.
- You may feel dizzy when you stand or sit up.
Mild dehydration means:
- You may be more thirsty than usual.
- You may pass less urine than usual.
Symptoms of serious illness may include:
- A severe headache.
- A stiff neck.
- Mental changes, such as feeling confused or much less alert.
- Extreme fatigue (to the point where it's hard for you to function).
- Shaking chills.
Here are some examples of possible changes in your usual pattern of headaches:
- Headaches are worse than usual.
- You get headaches more often.
- The pain is in a different area.
- The pain feels different.
- The medicines you usually take for headaches no longer seem to work.
Seek Care Now
Based on your answers, you may need care right away. The problem is likely to get worse without medical care.
- Call your doctor now to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care in the next hour.
- You do not need to call an ambulance unless:
- You cannot travel safely either by driving yourself or by having someone else drive you.
- You are in an area where heavy traffic or other problems may slow you down.
Seek Care Today
Based on your answers, you may need care soon. The problem probably will not get better without medical care.
- Call your doctor today to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care today.
- If it is evening, watch the symptoms and seek care in the morning.
- If the symptoms get worse, seek care sooner.
Make an Appointment
Based on your answers, the problem may not improve without medical care.
- Make an appointment to see your doctor in the next 1 to 2 weeks.
- If appropriate, try home treatment while you are waiting for the appointment.
- If symptoms get worse or you have any concerns, call your doctor. You may need care sooner.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Self-Care
Most of the time, headaches get better or go away with home treatment and don't require a visit to a doctor. Home treatment for headaches can often help reduce how long you have pain and how severe it is. Home treatment may also relieve other symptoms, such as a fever, nausea or vomiting, anxiety, or muscle aches. Start home treatment as soon as you can.
To treat a mild headache:
- Rest in a quiet, dark room.
- Place a cool compress on your forehead.
- Don't smoke, drink alcohol, or use illegal drugs.
- If your doctor has prescribed a specific treatment for your headaches, begin treatment as soon as a headache starts. Be sure to follow the doctor's instructions when you take any prescription medicine for your headache.
To reduce how often you get a headache, try:
- Relaxation exercises. These exercises can help take away tension and stress that cause headaches or make them worse.
- Heat, such as hot water bottles, heating pads, or hot baths. Heat can relax tense muscles. But be careful not to burn yourself.
- Ice, such as an ice pack applied to the back of the neck or the temples.
- Massage therapy, biofeedback, and other complementary medicine treatments. They can reduce muscle tension, especially in your neck and shoulder muscles. Muscle tension can cause headaches or make them worse.
To treat a child's headache:
- Talk to your child. Let your child know that you care. Extra attention and quiet time may be all that's needed to relieve the pain.
- If the doctor prescribed a specific treatment for the headaches, start treatment as soon as your child complains of the pain.
- Let your child rest quietly in a darkened room with a cool compress on their forehead.
- If your child's headache pain is mild, encourage your child to go on with normal activities.
- Let your child do any usual activities if your child feels like it, unless the headache pain is moderate to severe.
When to call for help during self-care
Call a doctor if any of the following occur during self-care at home:
- New or worse pain.
- New fever or vomiting.
- New or worse confusion or vision changes.
- Symptoms occur more often or are more severe.
Learn more
Watch
Preparing For Your Appointment
You can help your doctor diagnose and treat your condition by being prepared for your appointment.
Credits
Current as of: December 20, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: December 20, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.