Top of the pageCheck Your Symptoms
Swallowed or Inhaled Objects
Overview
When you swallow food, liquid, or an object, what is swallowed passes from your mouth through your throat, down your (esophagus), and into your stomach. A swallowed object will usually pass through the rest of your digestive tract without problems. It will show up in your stool in a few days. If food or a nonfood item gets stuck along the way, you may have pain when swallowing or trouble swallowing, even when swallowing your saliva. You may need medical care right away.
Sometimes when you try to swallow, the swallowed substance "goes down the wrong way." It gets breathed in to your windpipe or lungs (aspirated). This happens most often in children who are younger than 3 years and in adults who are older than age 50. When you breathe in (inhale) a substance, coughing is your body's normal response. It's the way your body tries to clear your throat and windpipe. The cough is helpful, and it may clear up the problem. Inhaling a substance into your lungs can cause lung inflammation and an infection (aspiration pneumonia).
The situation may be more serious when a person:
- Has signs of choking (complete airway obstruction). When the windpipe is blocked, air can't move in and out of the lungs. The person can't talk, cry, breathe, or cough. A blocked windpipe is a life-threatening emergency.
- The choking rescue procedure (Heimlich maneuver) is used to clear a blockage in adults and children older than 1 year.
- Back blows and chest thrusts are used in babies younger than 1 year.
- Has signs of a partially blocked windpipe. When the windpipe is partly blocked, some air can still move in and out of the lungs. The person may gag, cough, or have trouble breathing. Coughing will often pop out the food or object and relieve the symptoms. The choking rescue procedure is not recommended when the windpipe is partly blocked.
- Has an object stuck in the esophagus. Most swallowed objects pass through the digestive tract without any problem within a few days. But a swallowed object can scratch, irritate, or poke a hole in (puncture) the digestive tract.
- Has swallowed a poisonous object, such as a wild mushroom, a plant, or a chemical.
- Has swallowed a button disc battery, a magnet, or an object with lead. Batteries, magnets, and small objects with lead can be easily swallowed, especially by children. A disc battery that is swallowed can burn, corrode, or completely destroy tissue in the upper digestive tract. Magnets can stick to the bowel and cause a blockage or a hole to form. An object with lead may cause lead poisoning. If you think someone has swallowed a disc battery, do not cause vomiting. Call the National Battery Ingestion Hotline at 800-498-8666 right away and arrange for medical care.
- Swallowing 2 teaspoons of honey right away coats the battery and reduces damage to the esophagus.
- Two teaspoons of honey can be swallowed every 10 minutes for up to 6 doses.
- Note: Only give honey to a child older than 12 months and if the battery was swallowed in the past 12 hours.
- Has swallowed an object that doesn't come out in the stool within a few days.
About 80% to 90% of swallowed objects, like chewing gum, are harmless and pass through the digestive tract without problems. But some types of objects can cause more serious problems when they are swallowed. These objects include:
- Sharp objects, such as open safety pins, bones, toothpicks, needles, razor blades, or broken thermometers.
- Long objects.
- Large objects that may get stuck in the digestive tract and need to be removed.
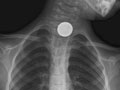
Your doctor may recommend tests such as an X-ray, endoscopy, or barium swallow. These tests can help find the object if it doesn't come out in the stool or if an inhaled object isn't coughed out. A special metal detector might be used. It can help locate a metal object, such as a coin, inside the body. Your doctor may then recommend a procedure to remove the object. Or your doctor may encourage you to keep checking the stool to be sure the object passes out of the body.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Check Your Symptoms
The medical assessment of symptoms is based on the body parts you have.
- If you are transgender or nonbinary, choose the sex that matches the body parts (such as ovaries, testes, prostate, breasts, penis, or vagina) you now have in the area where you are having symptoms.
- If your symptoms aren’t related to those organs, you can choose the gender you identify with.
- If you have some organs of both sexes, you may need to go through this triage tool twice (once as "male" and once as "female"). This will make sure that the tool asks the right questions for you.
Many things can affect how your body responds to a symptom and what kind of care you may need. These include:
- Your age. Babies and older adults tend to get sicker quicker.
- Your overall health. If you have a condition such as diabetes, HIV, cancer, or heart disease, you may need to pay closer attention to certain symptoms and seek care sooner.
- Medicines you take. Certain medicines, such as blood thinners (anticoagulants), medicines that suppress the immune system like steroids or chemotherapy, herbal remedies, or supplements can cause symptoms or make them worse.
- Recent health events, such as surgery or injury. These kinds of events can cause symptoms afterwards or make them more serious.
- Your health habits and lifestyle, such as eating and exercise habits, smoking, alcohol or drug use, sexual history, and travel.
Try Home Treatment
You have answered all the questions. Based on your answers, you may be able to take care of this problem at home.
- Try home treatment to relieve the symptoms.
- Call your doctor if symptoms get worse or you have any concerns (for example, if symptoms are not getting better as you would expect). You may need care sooner.
Blood in the stool can come from anywhere in the digestive tract, such as the stomach or intestines. Depending on where the blood is coming from and how fast it is moving, it may be bright red, reddish brown, or black like tar.
A little bit of bright red blood on the stool or on the toilet paper is often caused by mild irritation of the rectum. For example, this can happen if you have to strain hard to pass a stool or if you have a hemorrhoid.
A large amount of blood in the stool may mean a more serious problem is present. For example, if there is a lot of blood in the stool, not just on the surface, you may need to call your doctor right away. If there are just a few drops on the stool or in the diaper, you may need to let your doctor know today to discuss your symptoms. Black stools may mean you have blood in the digestive tract that may need treatment right away, or may go away on its own.
Certain medicines and foods can affect the color of stool. Diarrhea medicines (such as Pepto-Bismol) and iron tablets can make the stool black. Eating lots of beets may turn the stool red. Eating foods with black or dark blue food coloring can turn the stool black.
If you take aspirin or some other medicine (called a blood thinner) that prevents blood clots, it can cause some blood in your stools. If you take a blood thinner and have ongoing blood in your stools, call your doctor to discuss your symptoms.
Pain in adults and older children
- Severe pain (8 to 10): The pain is so bad that you can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain.
- Moderate pain (5 to 7): The pain is bad enough to disrupt your normal activities and your sleep, but you can tolerate it for hours or days. Moderate can also mean pain that comes and goes even if it's severe when it's there.
- Mild pain (1 to 4): You notice the pain, but it is not bad enough to disrupt your sleep or activities.
Pain in children under 3 years
It can be hard to tell how much pain a baby or toddler is in.
- Severe pain (8 to 10): The pain is so bad that the baby cannot sleep, cannot get comfortable, and cries constantly no matter what you do. The baby may kick, make fists, or grimace.
- Moderate pain (5 to 7): The baby is very fussy, clings to you a lot, and may have trouble sleeping but responds when you try to comfort him or her.
- Mild pain (1 to 4): The baby is a little fussy and clings to you a little but responds when you try to comfort him or her.
Symptoms of difficulty breathing can range from mild to severe. For example:
- You may feel a little out of breath but still be able to talk (mild difficulty breathing), or you may be so out of breath that you cannot talk at all (severe difficulty breathing).
- It may be getting hard to breathe with activity (mild difficulty breathing), or you may have to work very hard to breathe even when you’re at rest (severe difficulty breathing).
Severe trouble breathing means:
- You cannot talk at all.
- You have to work very hard to breathe.
- You feel like you can't get enough air.
- You do not feel alert or cannot think clearly.
Moderate trouble breathing means:
- It's hard to talk in full sentences.
- It's hard to breathe with activity.
Mild trouble breathing means:
- You feel a little out of breath but can still talk.
- It's becoming hard to breathe with activity.
Severe trouble breathing means:
- The child cannot eat or talk because he or she is breathing so hard.
- The child's nostrils are flaring and the belly is moving in and out with every breath.
- The child seems to be tiring out.
- The child seems very sleepy or confused.
Moderate trouble breathing means:
- The child is breathing a lot faster than usual.
- The child has to take breaks from eating or talking to breathe.
- The nostrils flare or the belly moves in and out at times when the child breathes.
Mild trouble breathing means:
- The child is breathing a little faster than usual.
- The child seems a little out of breath but can still eat or talk.
Disc batteries are small, round batteries used in toys, cameras, watches, and other devices. Because of the chemicals they can release, they can cause serious problems if they are swallowed or get stuck in an ear or the nose. Small magnets used in household items and objects that contain a lot of lead (such as bullets, buckshot, fishing weights and sinkers, and some toys) also can cause problems if swallowed.
- If a disc battery is stuck in the ear or nose:
- The battery needs to be removed right away—within 1 hour if possible.
- Use tweezers to try to remove the battery. If you can't remove it, get medical help.
- If you have swallowed a disc battery, magnet, or lead object:
- Get medical help right away.
- Do not try to vomit.
- Do not eat or drink anything.
Seek Care Today
Based on your answers, you may need care soon. The problem probably will not get better without medical care.
- Call your doctor today to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care today.
- If it is evening, watch the symptoms and seek care in the morning.
- If the symptoms get worse, seek care sooner.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Seek Care Now
Based on your answers, you may need care right away. The problem is likely to get worse without medical care.
- Call your doctor now to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care in the next hour.
- You do not need to call an ambulance unless:
- You cannot travel safely either by driving yourself or by having someone else drive you.
- You are in an area where heavy traffic or other problems may slow you down.
Self-Care
Here are some things you can do at home that help relieve discomfort after you swallow an object into your digestive tract.
- Don't cause (induce) vomiting.
It could cause you to inhale (aspirate) the object into your windpipe or lungs.
- Drink fluids.
If swallowing fluids is easy, try eating soft bread or a banana. If eating soft bread or a banana is easy, try adding other foods. Fruits, vegetables, and whole grains may help move the swallowed object through the digestive tract. Keep drinking more fluids until the object has passed in your stool. Extra fluid will help the object move through the digestive tract. The object should pass within a few days. Watch your stools to see if the object has passed. Don't use a laxative unless your doctor tells you to.
When to call for help during self-care
Call a doctor now or seek care if any of the following occur during self-care at home:
- New shortness of breath, wheezing, or moderate coughing.
- Can't swallow own saliva.
- Large amount of blood in vomit.
Call a doctor if any of the following occur during self-care at home:
- Mild shortness of breath, wheezing, or mild coughing.
- New or worse pain in the throat, chest, or belly.
- New or worse trouble swallowing.
- New vomiting or small amount of blood in vomit.
- New blood in the stool.
- The swallowed object does not pass in the stool within a few days.
- Symptoms occur more often or are more severe.
Learn more
Preparing For Your Appointment
You can help your doctor diagnose and treat your condition by being prepared for your appointment.
Credits
Current as of: October 19, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 19, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.