Diverticulitis
Condition Basics
What is diverticulitis?
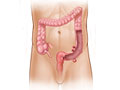
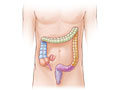
Diverticulitis is a condition that happens when pouches (diverticula) form in the wall of the colon and then become inflamed or infected. This can cause tenderness, cramps, or pain in the belly. Not everyone who has these pouches gets diverticulitis. Mild attacks may heal on their own.
What causes it?
Doctors aren't sure what causes diverticulitis. Bacteria grow in pouches (diverticula) that sometimes form in the wall of the colon. These bacteria can lead to inflammation or infection. Doctors think diverticula form when high pressure inside the colon pushes against weak spots in the colon wall.
What are the symptoms?
Belly pain, often in the lower left side, is the most common symptom of diverticulitis. The pain is sometimes worse when you move. Other symptoms include fever, chills, bloating, and gas. You may also have diarrhea or constipation. Symptoms can last from a few hours to several days, or longer if not treated.
How is it diagnosed?
To diagnose diverticulitis, your doctor will ask questions about your symptoms and examine you. You may have tests to see if you have an infection or other problems. The tests may include blood tests or a digital rectal exam. They may also include CT scans, ultrasound, or X-rays of your belly, or other tests.
How is diverticulitis treated?
Treatment for mild symptoms of diverticulitis starts with antibiotics, pain medicines, and diet changes. You can try home treatment, such as a heating pad, for pain. To treat serious symptoms, you may need a hospital stay or surgery.
Cause
Doctors aren't sure what causes diverticulitis. Bacteria grow in pouches (diverticula) that sometimes form in the wall of the colon. These bacteria can lead to inflammation or infection. Doctors think diverticula form when high pressure inside the colon pushes against weak spots in the colon wall.
It is not known why some people who have these diverticula get diverticulitis and others do not.
In most cases, a diet with good fiber makes stool that is bulky and can move easily through the colon. A low-fiber diet can cause small, hard stools. This means it takes more pressure in the colon to move stools out of the body. This puts more pressure on the walls of the colon.
What Increases Your Risk
The possibility of having diverticulitis increases with age.
You may be more likely to develop diverticulitis if you:
- Eat a low-fiber diet.
- Have a family history of diverticulosis.
- Use nonsteroidal anti-inflammatory drugs (NSAIDs) or aspirin regularly (more than 4 days a week) for many years.footnote 1
Symptoms
Symptoms of diverticulitis include:
- Tenderness, cramps, or pain in the belly. This is often in the lower left side but may occur on the right. These symptoms are sometimes worse when you move. Pain is the most common symptom.
- Fever and chills.
- A bloated feeling, swelling in the belly, or gas.
- Diarrhea or constipation.
- Nausea and sometimes vomiting.
- Not feeling like eating.
Symptoms may last from a few hours to several days. They may last longer if the problem isn't treated. Complications also can cause symptoms. If an abnormal opening (fistula) develops between the colon and the vagina or the colon and the urethra, you may pass air or stool from the vagina or the urethra.
What Happens
Diverticulitis occurs when pouches (diverticula) that have formed in the wall of the large intestine (colon) become inflamed or infected. It is not known why some people who have these pouches (diverticulosis) develop diverticulitis and others do not.
Mild attacks of diverticulitis, with few symptoms of infection or inflammation, sometimes heal without treatment. In most cases, doctors prescribe oral antibiotics. They may also suggest a clear liquid diet to rest the bowel until it isn't inflamed.
When infection and symptoms are severe, diverticulitis is treated in the hospital. Treatment includes antibiotics given in a vein (I.V.) and resting the bowel with I.V. fluids. If symptoms are severe and not treated, problems such as an abscess or fistula may happen. Surgery often is needed to treat these.
It is common to have lower belly pain after recovering from an attack of diverticulitis. But this pain doesn't always mean it's returned.
When to Call
Call 911 or other emergency services immediately if the person:
- Is bleeding from the anus and has signs of shock, such as:
- Passing out (losing consciousness).
- Feeling very dizzy, weak, or less alert.
Call your doctor now if you have:
- Belly pain. This is usually in the lower left side. It is sometimes worse when you move.
- Fever or chills.
- Nausea and vomiting.
- Unusual changes in your bowel movements.
- Bloating and gas.
- Blood in your stool.
Call your doctor if you:
- Have cramping pain that does not get better when you have a bowel movement or pass gas.
- Have been losing weight without trying.
Call your doctor if you are treating mild diverticulitis at home and:
- You have a fever.
- Your pain is getting worse.
- You can't keep down liquids.
- You are not better after 3 days.
Check your symptoms
Exams and Tests
To diagnose diverticulitis, your doctor will ask questions about your symptoms and examine you. The doctor may do tests to see if you have an infection or to make sure that you don't have other problems. Tests may include:
- Blood tests, such as a complete blood count (CBC).
- Other tests, such as a CT scan, ultrasound, MRI, or X-ray of your belly. These may help find the cause of belly pain and other symptoms.
- A digital rectal exam. This looks for tenderness or a mass in the lower pelvic area.
- A fecal occult blood test. This looks for blood in your stool.
- Flexible sigmoidoscopy and colonoscopy. These may be done if you have bleeding or to look for narrow spots or growths in the bowel.
Learn more
Treatment Overview
Treatment depends on how bad your symptoms are. If the pain is mild, you are able to drink liquids, and you have no signs of complications, treatment may include:
- Medicines such as antibiotics and pain relievers.
- Changes in diet. These changes start with a clear-liquid or bland diet that is low in fiber. You follow this diet until the pain goes away. You then increase how much fiber you eat.
If the pain is severe, you are not able to drink liquids, or you have complications of diverticulitis, you may need a hospital stay. Treatment will include:
- Antibiotics given in a vein (intravenous, or I.V.).
- Fluids and food given through your vein only (no food or drink by mouth) for up to a week. This allows the bowel to rest.
Sometimes surgery is needed to treat some problems or repeated attacks.
Self-Care
- Drink plenty of fluids. If you have kidney, heart, or liver disease and have to limit fluids, talk with your doctor before you increase the amount of fluids you drink.
- Stay with liquids or start with small amounts of food until you are feeling better. Then you can return to regular foods and slowly increase the amount of fiber in your diet.
- Get extra rest until you are feeling better.
- Be safe with medicines. Read and follow all instructions on the label.
- If the doctor gave you a prescription medicine for pain, take it as prescribed.
- If you are not taking a prescription pain medicine, ask your doctor if you can take an over-the-counter medicine.
- If your doctor prescribed antibiotics, take them as directed. Do not stop taking them just because you feel better. You need to take the full course of antibiotics.
- Do not use laxatives or enemas unless your doctor tells you to use them.
Learn more
Credits
Current as of: October 19, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 19, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.