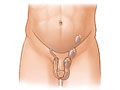
Undescended Testicle
Conditions Basics
What is an undescended testicle?
As a baby boy grows inside his mother, he develops testicles. Early in his development, his testicles are in his belly. Normally, before he is born, his testicles move down into his scrotum, the sac that hangs below the penis. When one testicle does not move into the scrotum as it should, the baby has an undescended testicle. In rare cases, both testicles are undescended.
It is most common in baby boys who were born before their due date or who were very small at birth.
Most of the time, the testicle descends (drops) on its own by the time the baby is 3 months old. If your baby's testicle hasn't dropped by the time he is 6 months of age, your doctor may suggest treatment.
What causes it?
Doctors don't really know what causes an undescended testicle. This common condition runs in some families (can be inherited).
What are the symptoms?
An undescended testicle doesn't cause pain or other symptoms. The scrotum may look a little smoother or less developed on one side, or the side without a testicle may look smaller and flatter. You can't feel the testicle in the scrotum on the side where it hasn't descended.
How is it diagnosed?
At newborn and well-baby visits, your doctor will check your baby's scrotum.
- If the testicle can be felt but it is not in the scrotum, the doctor will probably want to check your baby again at 3 to 6 months of age. By this time, the testicle may have moved into place on its own.
- Sometimes the doctor can't feel the testicle at all. It could still be in the baby's belly, it could be too small to feel, or it could be absent. The doctor may recommend a type of surgery called laparoscopy to see if he or she can find the testicle. Laparoscopy requires only a small cut below the belly button, which heals quickly.
- If both testicles are undescended and can't be felt in the groin, the doctor will do a blood hormone test to find out if the testicles are absent. This means having no testicles at all. It is very rare to have two absent testicles.
Some other conditions are closely related to undescended testicles, such as an ectopic or retractile testicle. In both of these conditions, the testicle is in an abnormal position in the groin or scrotum. Your doctor will take care to make the correct diagnosis so your child can get the right treatment.
How is an undescended testicle treated?
Usually doctors recommend a wait-and-see approach for newborns. If the testicle hasn't dropped on its own within 6 months, your doctor may recommend surgery (orchiopexy or orchidopexy). Surgery is usually recommended by the time the baby is 18 months old.footnote 1 It is safe and effective and has few risks. Most babies recover quickly.
When babies have a testicle that can't be felt, doctors may do a different surgery that needs only a small cut (laparoscopy).
Why is it important to treat it?
Treatment is important because having an undescended testicle increases the risk of:
- Infertility. Damage to a testicle's sperm-making ability can begin as early as 12 months of age. That's why many doctors advise treating an undescended testicle by the time a baby is 1 year old and no later than age 2. Treatment helps lower the chance of infertility.
- Cancer of the testicles. Men who were born with undescended testicles have a higher rate of testicular cancer than other men. But this cancer is rare. It can be cured if found early. If you are a young man who was born with an undescended testicle, talk with your doctor about what you should do.
Credits
Current as of: November 15, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: November 15, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.