Hemodialysis
Treatment Overview
Chronic kidney disease and acute kidney injury (also known as acute renal failure) cause the kidneys to lose their ability to filter and remove waste and extra fluid from the body. Hemodialysis is a process that uses a man-made membrane (dialyzer) to:
- Remove wastes, such as urea, from the blood.
- Restore the proper balance of electrolytes in the blood.
- Get rid of extra fluid from the body.
Hemodialysis for acute kidney injury may be done daily until your kidneys are working again.
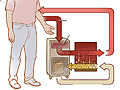
You are connected to a filter (dialyzer) by tubes attached to your blood vessels. Your blood is slowly pumped from your body into the dialyzer, where waste products and extra fluid are removed. The filtered blood is then pumped back into your body.
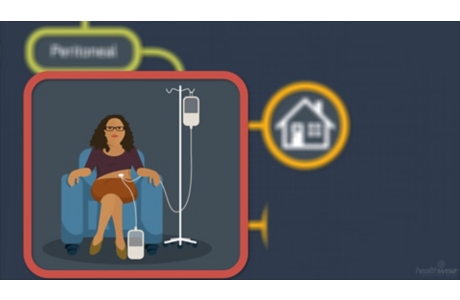
There are different types of hemodialysis. It can be done in a hospital or center or at home. If it's at home, you do the dialysis yourself, often with the help of a friend or family member. You have choices for how long and how often you do it. You can also do it overnight. Talk about these with your doctor to decide which one might be best for you.
Access
Before treatments can start, your doctor will need to create a site where the blood can flow in and out of your body during the dialysis sessions. This is called the dialysis access. The type of dialysis access you have will depend in part on how quickly you need to start dialysis.
There are different types of access for hemodialysis:
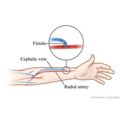
- A fistula connects an artery to a vein in your arm. It may take several months to form.
- A graft is a small tube that connects the artery and vein. It doesn't last as long as a fistula.
- A venous catheter is a tube placed in your neck or chest. It's used for a short time only.
Things to consider
- Hemodialysis is done mainly by trained health workers. They can watch for problems.
- You can do it at a center where other people are doing dialysis. This can help provide emotional support.
- You can schedule your treatments in the evenings and maybe at home. This gives you more control over your schedule.
- It usually needs to be done on a set schedule at least 3 times a week.
- It can cause side effects, such as low blood pressure and muscle cramps. These can often be treated easily.
- It requires being poked by a needle at each treatment. This bothers some people. Others get used to it and can do it themselves.
What To Expect
About once a month, you will have blood tests to make sure you are getting the right amount of hemodialysis. These tests are done to help find out how well hemodialysis is working. Your weight before and after each session will be recorded, as will the length of time it takes to complete the dialysis session. If you have hemodialysis at home, you will need to keep records of your weight before and after each session and the length of each session.
Learn more
Why It Is Done
Hemodialysis is often started after symptoms or complications of kidney failure develop. These may include:
- Symptoms of uremic syndrome, such as nausea, vomiting, loss of appetite, and fatigue.
- Mild confusion.
- Signs of the kidneys' inability to rid the body of daily excess fluid intake, such as swelling.
- High levels of potassium in the blood (hyperkalemia).
- High levels of acid in the blood (acidosis).
Hemodialysis is sometimes used when acute kidney injury develops. Dialysis is always used with extra caution in people who have acute kidney injury, because dialysis can sometimes cause low blood pressure, irregular heart rhythms (arrhythmias), and other problems that can make acute kidney injury worse.
How Well It Works
Hemodialysis does not fully replace normal kidney function. It doesn't reverse chronic kidney disease or kidney failure. Hemodialysis only provides up to 10% of normal kidney function. For this reason, it's important to take your medicines as instructed and follow your eating plan.
Dialysis is sometimes used to treat an acute kidney injury. It may be used when fluid and electrolyte problems are causing severe symptoms or other problems. Some people who develop acute kidney injury stay dependent on hemodialysis and will go on to develop kidney failure.
Risks
Most complications that occur during dialysis can be prevented or easily managed if you are monitored carefully during each dialysis session. Possible complications may include:
- Low blood pressure (hypotension). This is the most common complication of hemodialysis.
- Muscle cramps.
- Irregular heartbeat (arrhythmia).
- Nausea, vomiting, headache, or confusion (dialysis disequilibrium).
- Infection, especially if a central vascular access device (CVAD) is used for hemodialysis.
- Blood clot (thrombus) formation in or near the CVAD.
- Technical complications, such as trapped air (embolus) in the dialysis tube.
Long-term complications of dialysis may include:
- Inadequate filtering of waste products (hemodialysis inadequacy).
- Blood clot (thrombus) formation in the dialysis graft or fistula.
- Cardiovascular disease (heart disease, blood vessel disease, or stroke).
Credits
Current as of: October 11, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 11, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.